Daijiworld Media Network – New York
New York, Apr 21: A recent medical case has highlighted the diagnostic challenges of Gonococcal endocarditis, a rare but aggressive infection, underscoring the importance of detailed patient history and advanced diagnostic tools.
The condition, caused by the bacterium Neisseria gonorrhoeae, can present as a severe, culture-negative infection with complications such as embolism and rapid destruction of heart valves.
According to a recently published case report, a 53-year-old man was admitted after suffering a ventricular fibrillation arrest linked to a heart attack and acute headache. Further evaluation revealed a systolic murmur and a large vegetation on the mitral valve detected through echocardiography. Brain imaging showed multiple infarcts, while chest scans suggested septic emboli.
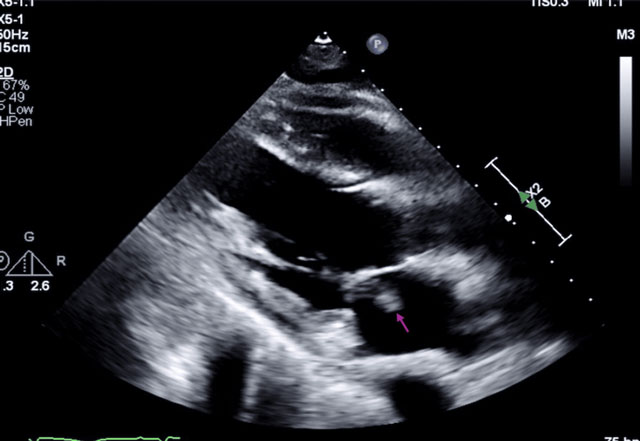
Despite strong clinical signs of Infective endocarditis, blood cultures remained negative, complicating the diagnosis. The patient was initially treated with antibiotics including ceftriaxone and vancomycin. However, due to extensive valve damage and embolic complications, he required mitral valve replacement surgery.
A definitive diagnosis was achieved only after advanced molecular testing. Polymerase chain reaction (PCR) analysis of the excised valve tissue identified Neisseria gonorrhoeae as the causative organism. The patient was subsequently treated with azithromycin and a six-week course of ceftriaxone.
Doctors later obtained additional history revealing multiple sexual partners, lack of routine screening for sexually transmitted infections, and inconsistent use of protection. The report noted that such details are often overlooked during initial assessments, especially when the source of infection is unclear.
Experts emphasised that gonococcal endocarditis, though rare, is highly virulent and can progress rapidly, often necessitating surgical intervention. Its tendency to present as a culture-negative infection makes diagnosis particularly challenging using conventional methods.
The case underlines the need for clinicians to consider uncommon pathogens in severe or atypical presentations and to incorporate comprehensive sexual history into routine evaluation. It also highlights the growing role of molecular diagnostics in identifying elusive infections and guiding timely treatment.